|
Trauma must be differentiated from other kinds of stressful events and conceptualized as an incident defined by physical injury rather than by emotional response. Discerning the critical distinctions required to understand PTSD depends on underlying clarity in terminology and precision in application of the diagnosis by academicians and clinicians. Research findings related to specific changes in the editions were provided from available research literature identified through specific PubMed searches using keywords relevant to each specific change.įundamental topics of debate identified in this review are validity of the diagnosis, the trauma criterion, the role of symptoms in defining its psychopathology, differentiation from other disorders, and specifiers such as delayed onset.ĭSM-5 has corrected several major ambiguities and errors of the former editions that are fundamental to the construct of PTSD as a disorder that is defined conditionally in relation to exposure to trauma, but problems remain in DSM-5 trauma criteria, especially inconsistencies between exposure criteria and the definition of trauma. 
For some women, the problematic change in orgasm occurred. The symptom must last for at least six months and not be related to other physical, mental or relational problem. The DSM-5 explains that these changes can be reduced intensity, delay, infrequency or absence of orgasm. Sections of the criteria and accompanying text were sorted into tables permitting visual comparisons across the editions. Female orgasmic disorder is marked by a significant change in orgasm. This article chronicles the evolution of PTSD across editions of the DSM.ĭiagnostic precursors to PTSD in DSM-I and DSM-II were briefly described, followed by systematic review of PTSD in subsequent editions of the DSM. No reviews have fully documented the shifting PTSD definitions across editions of the criteria. This article is a US Government work and is in the public domain in the USA.The diagnosis of posttraumatic stress disorder (PTSD) has remained controversial from the time of its first inclusion in DSM-III. Finally, the very different approaches taken by DSM-5 and ICD-11 should have a profound effect on future research and practice. The preschool subtype incorporates important developmental factors affecting the expression of PTSD in young children. The dissociative subtype may open the way to a fresh approach to complex PTSD. In DSM-5, it has moved beyond a narrow fear-based anxiety disorder to include dysphoric/anhedonic and externalizing PTSD phenotypes. Specific issues discussed about the DSM-5 PTSD criteria themselves include a broad versus narrow PTSD construct, the decisions regarding Criterion A, the evidence supporting other PTSD symptom clusters and specifiers, the addition of the dissociative and preschool subtypes, research on the new criteria from both Internet surveys and the DSM-5 field trials, the addition of PTSD subtypes, the noninclusion of complex PTSD, and comparisons between DSM-5 versus the World Health Association's forthcoming International Classification of Diseases (ICD-11) criteria for PTSD. The rationale is presented that led to the creation of the new chapter, "Trauma- and Stressor-Related Disorders," within the DSM-5 metastructure. In 2013, the American Psychiatric Association revised the PTSD diagnostic criteria in the 5 th edition of its Diagnostic and Statistical Manual of Mental Disorders (DSM-5 1).PTSD was included in a new category in DSM-5, Trauma- and Stressor-Related Disorders. The process is described in this article. 
There was a high threshold for any changes in any DSM-IV diagnostic criterion. DSM-5 American Psychiatric Association ) was empirically based and rigorous. 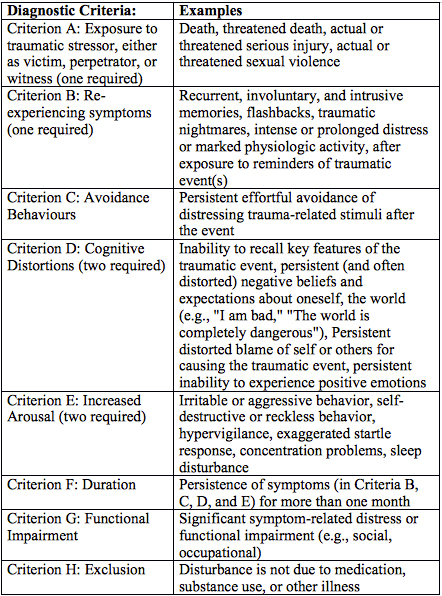
The process that resulted in the diagnostic criteria for posttraumatic stress disorder (PTSD) in the Diagnostic and Statistical Manual of Mental Disorders (5th ed.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
